Here to provide you with world-class care.
Whether you’re looking for a world-class hospital, local primary care physician, specialty services like orthopaedics, convenient urgent care clinics, and so much more…Williamson Health provides the top-tier care you need, close to your home.


ABOUT US
We know Williamson County.
As this community has grown, so have we. What started as a single building called Williamson County Hospital in 1958 has grown into a regional health system, and we are proud to be poised to take care of our communities for generations to come. The entire Williamson Health organization is committed to providing world-class care that feels like home.
You can stay right here in Williamson County to get excellent care that meets all your needs. Williamson Health makes it possible.
Our Awards
Growing with Williamson County for 65+ years.
Here to provide you with world-class care.
Whether you’re looking for a world-class hospital, local primary care physician, specialty services like orthopaedics, convenient urgent care clinics, and so much more…Williamson Health provides the top-tier care you need, close to your home.

ABOUT US
We know Williamson County.
As this community has grown, so have we. What started as a single building called Williamson County Hospital in 1958 has grown into a regional health system, and we are proud to be poised to take care of our communities for generations to come. The entire Williamson Health organization is committed to providing world-class care that feels like home.
You can stay right here in Williamson County to get excellent care that meets all your needs. Williamson Health makes it possible.

Our Awards



Growing with Williamson County for 65+ years.
FOCUSED CARE
World-class services for every healthcare need.
No matter what type of care you’re looking for, Williamson Health combines highly-skilled healthcare providers, innovative facilities and state-of-the-art technologies to provide exceptional healthcare to our region.
Our board-certified family and internal medicine physicians focus on prevention and wellness, the diagnosis and treatment of both common and complex diseases and management of chronic conditions.
Our nationally recognized surgery department is committed to providing advanced surgical care and treatment options that suit your unique needs. From diagnosis to treatment and recovery, our team of trusted surgical experts and dedicated staff puts you first.
Whether you are seeking care due to aging or overuse, a traumatic accident or sports-related injury, our team of experts work with you every step of the way to help improve your range of motion, mobility and quality of life.
Williamson Health provides expert cardiology treatment from ambulance to recovery. Our highly advanced EMS can detect a heart attack and digitally transmit information to our ER, and our chest pain center and accredited cardiac and pulmonary rehabilitation program are unmatched.
Trusted partners
expanding care.
From our award-winning hospital, Williamson Medical Center, to our state-of-the-art breast health center, premier orthopaedic health center, strategically located physician practices across the county and more, you'll find top-tier care for any need – right around the corner.
Williamson Health includes...
![VHWMC_WIC (revised)[1] VHWMC_WIC (revised)[1]](https://williamsonhealth.org/content/uploads/2023/06/VHWMC_WIC-revised1.jpeg)
...and so much more!
World-class care that feels like home
“I don't think I've ever had a better hospital experience. An experience where literally *every* staff person was kind to us, and genuinely wanted to support the recently moved, worried mom, who showed up in the middle of the night, with a very sick baby, and no family or friends to call.”
Kristee B., Williamson County Parent
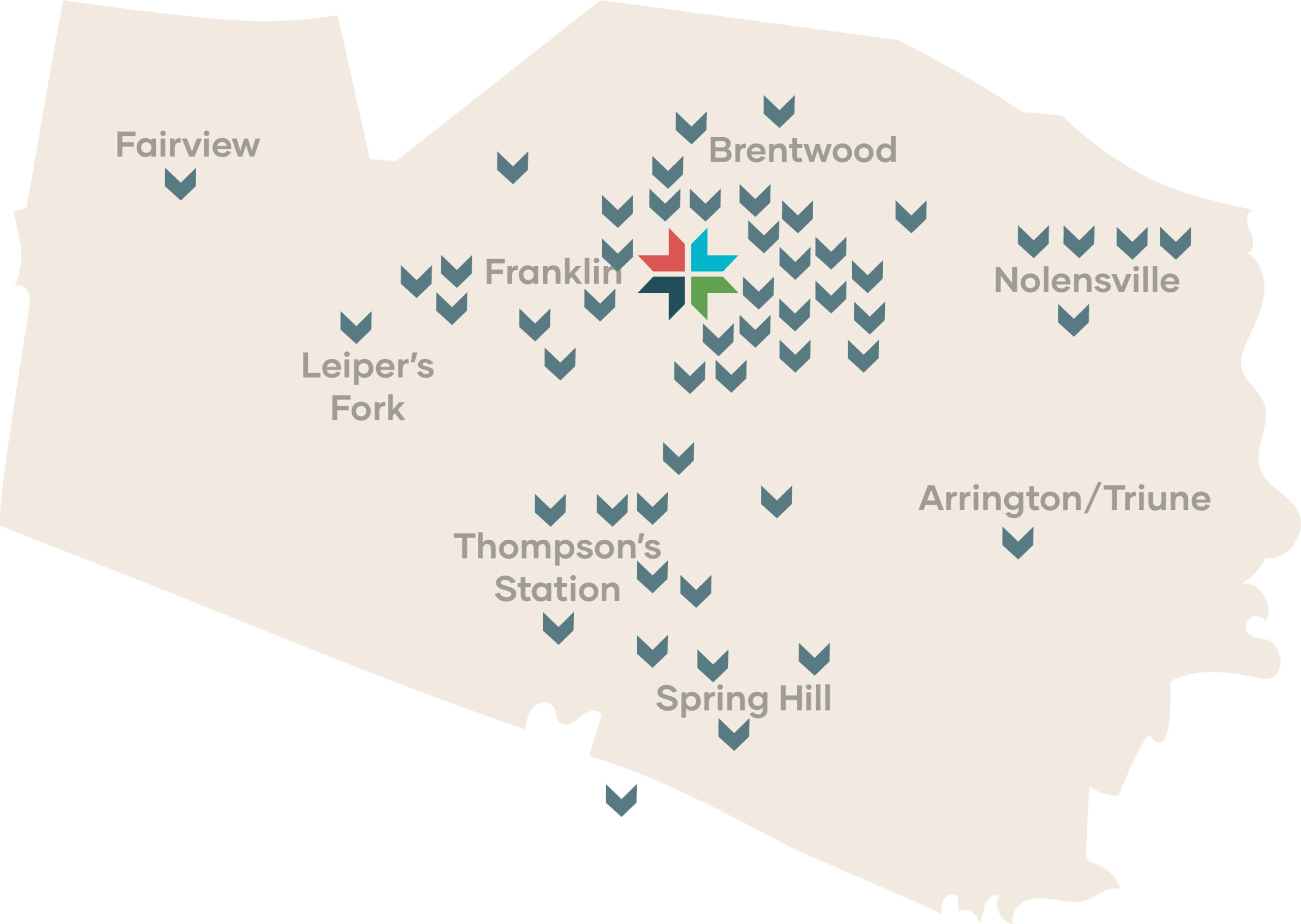
World-class care close to home
Whether you’re in Brentwood, Franklin, Spring Hill, Nolensville, Fairview, Thompson’s Station, Leiper’s Fork or anywhere in between, you’ll find the excellent care you need nearby at Williamson Health.
ANNOUNCEMENT
Williamson Health announces historic expansion to facilities and services.
Williamson Health is already a premier healthcare system providing high-quality care. As Williamson County and the surrounding region continue to grow, it’s imperative that Williamson Health do the same. We are committed to providing the highest quality healthcare to the communities we serve, and these world-class additions and renovations will allow us to continue doing so for years to come.
This ambitious project will touch nearly every department of our flagship hospital, with improvements coming to Labor & Delivery, Neonatal Intensive Care Unit, Cardiology, Surgery, Emergency Services, Intensive Care Unit and more.
