News
What's going on across Williamson Health? You've come to the right place! Stay up to date with the latest information from Williamson Health including stories of world-class care, awards, news and more.
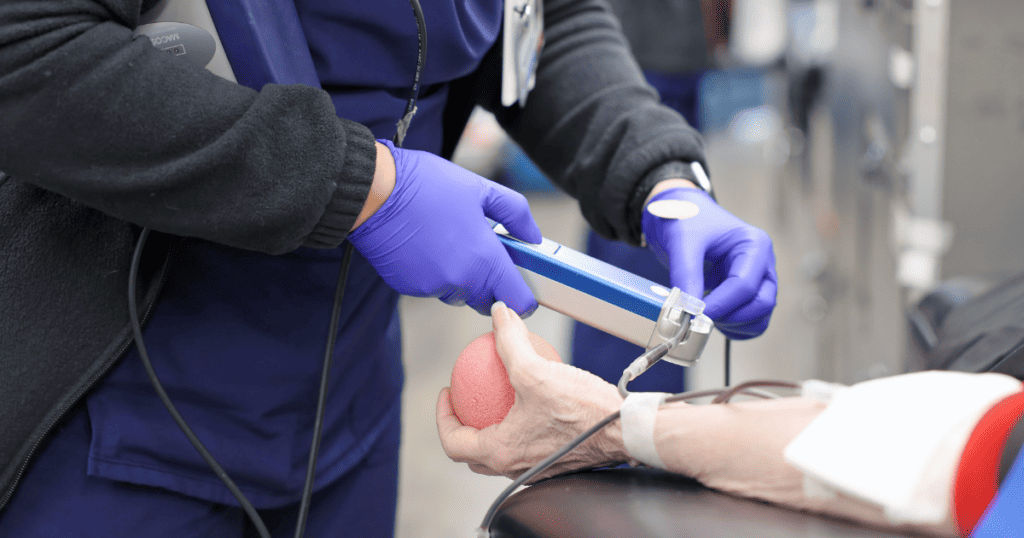
Two Opportunities in April to Give Blood Ahead of Severe Weather Season
Blood donors can choose between two dates this month to help save lives in Williamson County. Williamson Health and Bone…
Williamson Health, Bone and Joint Institute Expanding Healthcare Services in Spring Hill
As a testament to their mission of delivering high-quality and compassionate care to the communities they proudly serve, Williamson Health…
Embracing Spring: Occupational Therapy Month and the Benefits of Gardening
Spring is the perfect time to get outdoors, and gardening can be a great way to enjoy nature while reaping…
Williamson Health, Bone and Joint Institute Earn 3 FranklinIs Sizzle Awards
For the second year in a row, Williamson Health has won the award for Best Health & Wellness in the…
Lacrosse The Country: Looking At The Game From A Player Turned Physician
Originally published in the Williamson Herald — A new sports phenomenon is taking the Southeast by storm. Whether you’re a high school…
Empowering Women Through Pelvic Health Solutions with Dr. Jennifer Tatalovich
Originally published in Williamson County Living — Pelvic health issues aren’t the easiest subjects to talk about, but Jennifer Tatalovich, M.D., wants to…
Shoulder Injuries Across Various Age Groups with Dr. Todd Wurth
Originally published in the Williamson Herald — Whether you’re prepping for your senior season of high school tennis or kicking off…
American Heart Month Blood Drive Set for February 27
Williamson Health and Bone and Joint Institute of Tennessee are partnering with Blood Assurance, the sole provider of blood products…
When A Heart Attack Strikes, Minutes Matter
Minutes Matter – when a heart attack strikes, it’s critical to act quickly. Fast medical treatment can drastically improve your…
Empowering Heart Health with Dr. Brian Long
Originally published in Williamson County Living — February is American Heart Month, and it’s the perfect time to take steps to improve…